INTRODUCTION
According to the Korean National Statistical Office in 2009, the mortality rate for cerebrovascular disease and heart disease came in 2nd and 3rd, respectively, next only to cancer.
1) Thus, control of chronic diseases such as hypertension, diabetes, and hypercholesterolemia is emphasized in public health. Of them, lipid lowering therapy significantly reduces the incidence and mortality rate for cardiovascular disease (CVD) in patients with hypercholesterolemia.
2,3) Therefore, the National Cholesterol Education Program Adult Treatment Panel (NCEP-ATP) III guidelines encouraged to lower the target level of cholesterol.
4)
Rosuvastatin has a strong potency among several lipid lowering drugs, but has a relatively low lipophilicity and good safety.
5) In addition, it is known to reduce CVD mortality when used as the primary preventative treatment in patients with low CVD risk.
5) As most of the patients visiting primary care physicians are hypercholesterolemic patients with low CVD risk, this study was conducted with rosuvastatin, whose effects on primary prevention had been previously reported.
In order to obtain the goal of lipid reduction, the compliance of patients to the drugs is important, but it is commonly overlooked. The compliance was especially low in the case of chronic diseases compared to acute diseases.
6) A previous study reported that the compliance of patients with hypercholesterolemia tended to decrease rapidly six months after the start of treatment.
6) In addition, lipid lowering therapy in primary care mostly aims for the primary prevention of CVDs, and it was reported that the discontinuation of drugs was higher in the primary prevention than in the secondary prevention.
2,7-10) Also previous studies reported that the lipid lowering drugs were continuously taken for a long time in only about 50% of cases.
11,12)
However, there have been only a few studies on related factors among the studies on compliance of lipid lowering therapy.
13-17) Therefore, we aimed to observe the compliance to rosuvastatin of patients with hypercholesterolemia in the primary care setting and to check the factors related to drug compliance by examining sociodemographic characteristics, previous statin use, and health related factors.
DISCUSSION
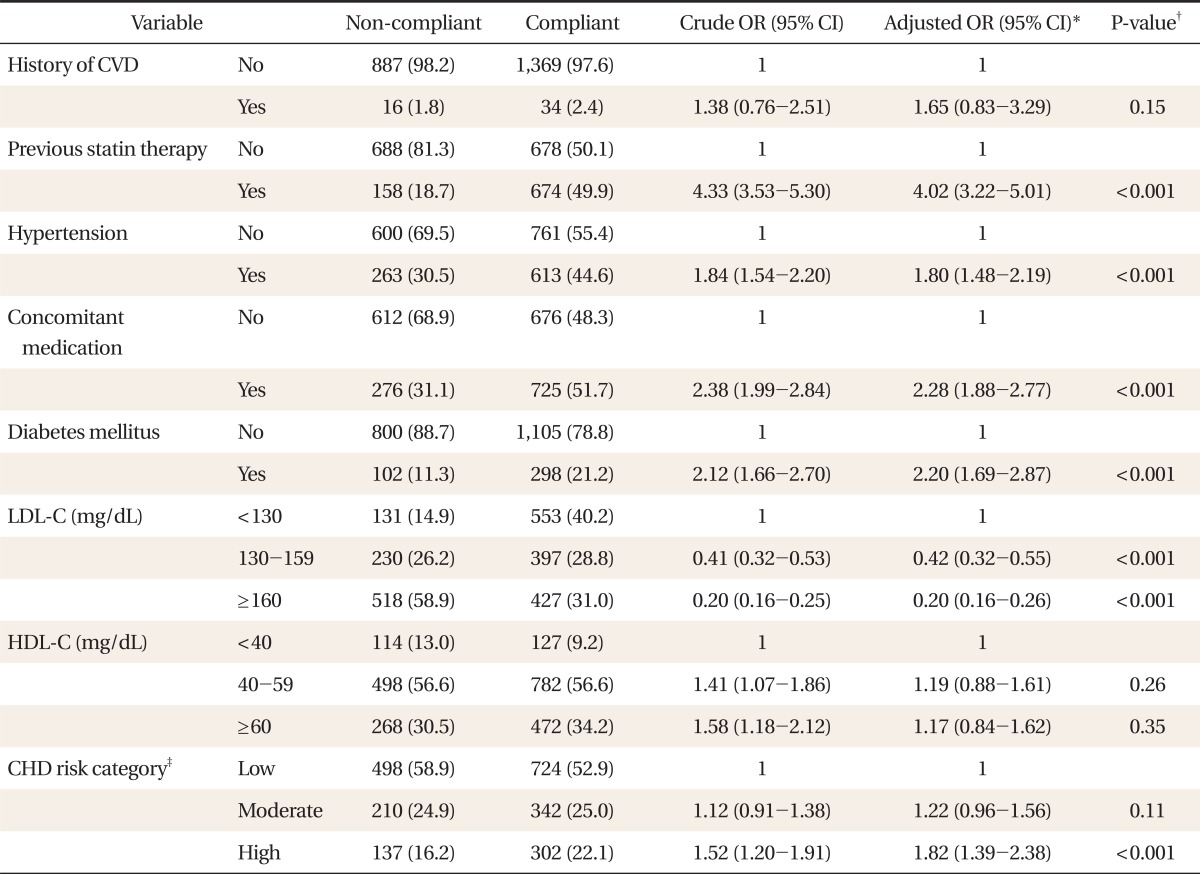
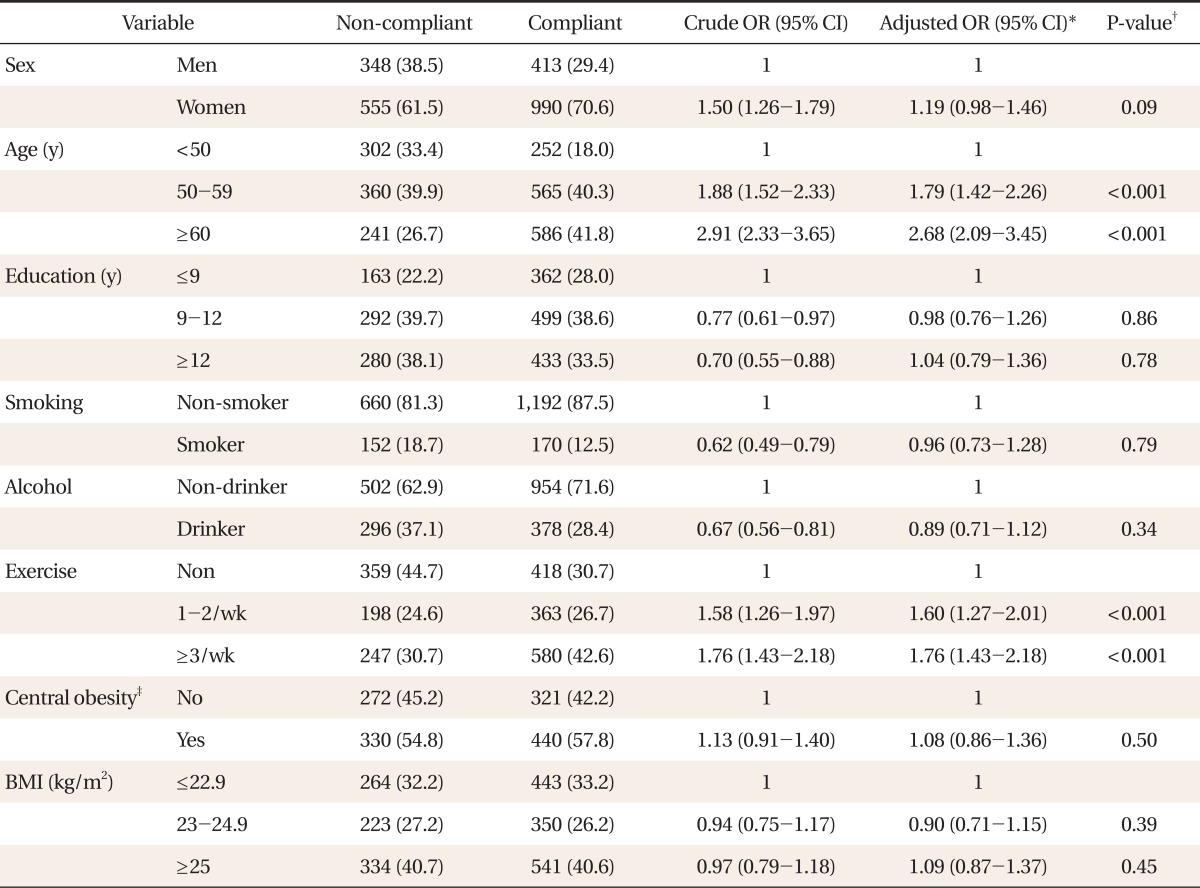
This study investigated the compliance of patients receiving lipid lowering therapy at a primary care facility during a treatment period of 24 weeks and examined the factors related to the compliance. As a result of analysis, age, frequency of exercise, existence of hypertension and diabetes, presence or absence of concomitant medication, whether the patient had been taking statin previously, level of LDL cholesterol, and CHD risk category were the factors related to the compliance with lipid-lowering therapy.
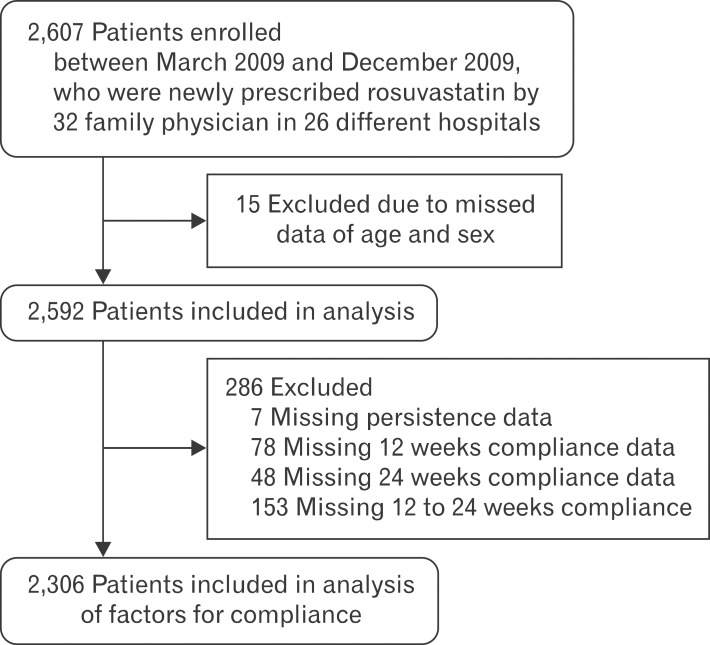
The ratio of compliance in the present study was 54.1%, and similar results were shown in previous studies.
8,12,17) The adherence was 72%, which was similar to results in the primary prevention clinical trial (69% to 71%)
2) and lower than the results in the secondary prevention clinical trial (81% to 90%).
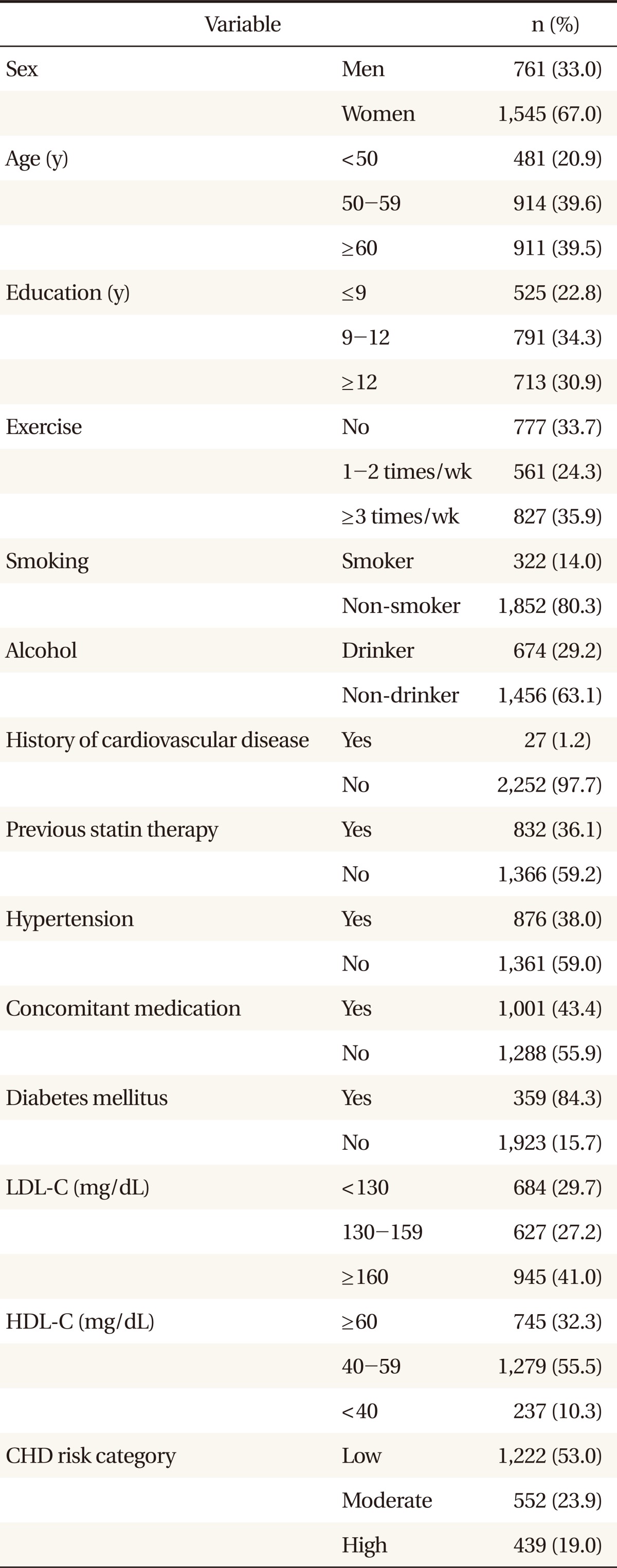
8,9) The patients who had had a CVD previously were included in this study, but they occupied only 2.2%. Thus, previous CVD history might not have affected the compliance in this study.
The results of this study indicate that the greater the age of the patient, the greater the compliance; i.e., younger patients do not take statins diligently. Most previous studies also showed similar results.
13,15,17) In our study, there was no difference in compliance according to sex, and this was similar with previous studies,
8,12,13) but a few studies did report that women had a lower compliance.
15) Patients who exercised more frequently had higher compliance and similar results were shown in other studies.
13,17) This could mean that those who exercise more had more interest in health and better health behavior. Smoking was a factor of low compliance in other studies,
13,17) but, in the present study, it was identified that there was no difference in compliance depending on smoking along with drinking status. As the ratio of women in the subjects of this study was 66.6%, which comes under two-thirds, and thus the smoking rate was 14.8% and the drinking rate was 31.9%, which were much lower than the average rates of Korean adults. Hence there is a possibility that this result was drawn due to selection bias.
The compliance was markedly higher in the group that had been taking statin previously than in the group that started taking statin for the first time (OR, 4.02). This was similar to results of previous studies,
13,15,17) but there were also a few studies showing conflicting results.
8) In our study, the compliance was significantly higher in participants with hypertension or diabetes, and there was no relationship in patients with CVD. In previous studies, the compliance was significantly higher in patients with hypertension, diabetes or cardiovascular diseases,
12,15) and also there were several studies with no relationship.
17) In our study, as participants with CVD occupied only 2.2% and most participants were mainly in primary prevention, CVD could not be related with compliance. In addition, compliance was significantly higher in participants with concomitant medications (OR, 2.28), and this was similar in previous studies.
18) The reason for the low compliance in the group of patients taking rosuvastatin only may be that these patients had fewer effects of treatment or symptoms, and, they may lack the motivation for taking rosuvastatin regularly and the knowledge of chronic diseases.
18)
In the present study, it was identified that the higher the level of LDL cholesterol, the lower the compliance. Several studies reported that the higher the total cholesterol before starting the treatment, the lower the compliance, but it was not statistically significant,
13,17) and the relationship between the level of LDL cholesterol and the compliance has never been discussed. It is thought that the negative correlation with the compliance was shown in this study because when the CHD risk level is higher, the treatment is started at a lower level of LDL cholesterol. Actually, as a result of linear analysis between the LDL cholesterol and CHD risk category, the P-value was 0.014, showing a negative correlation. That is, the group with lower LDL cholesterol is the group with higher CHD risk level. It was found that the compliance was significantly higher when the CHD risk level was higher, and the two results coincide with each other.
There are several methods to measure compliance, which include examination of daily record, represcription rate, pill count, and electronic medication monitor.
19) In this study, physicians checked the drug compliance, the continuance of rosuvastatin, and outpatient clinic visits during the follow-up period. Therefore, compliance would be measured better than that of other studies that examined only the continuance of treatment. However, as this study depended on the responses of patients for drug compliance, it may be influenced by the wrong reports of patients more than pill count or electronic medication monitor. However, our method is a cheap and easily used method which is actually used much in primary care, and thus it seems that there would be no great obstacle in the evaluation of compliance.
Another limitation is that the present study did not follow-up the compliance after 24 weeks. However, in starting the first drug treatment, changes in compliance is sharp within the first 6 months, and shows a mild decrease after that, and thus it can be seen that there is sufficient significance in the evaluation of compliance. This study targeted patients who visited the department of family medicine of hospitals, and thus it may be difficult to apply it to all the hypercholesterolemic patients in Korea. Despite these limitations, the present study demonstrates significance in that it identified the compliance of lipid lowering therapy in primary care with the main purpose of primary prevention and the factors influencing compliance.
In addition, this study added drug compliance to the evaluation of compliance, assessed the CHD risk category together, and investigated a large population. It is known that in order to increase compliance, various attempts should be integrated such as increasing the degree of participation of patients in treatment through various methods including education, self-monitoring using devices, reminding the patients to take the medicine, performing a telephone consultation, reminding by phone or letter, or prescribing to take the medicine once daily.
20) As identified in this study, the compliance of patients without chronic diseases such as diabetes or hypertension was low and patients younger than 50 years receiving the single treatment of lipid lowering agent showed low compliance. Therefore, it is necessary to emphasize the importance of taking the lipid lowering agent and to conduct education on risks of CVDs. Moreover, drug compliance could be increased by life style modifications such as regular exercise and monitoring the patients through diverse approaches including telephone use.
In conclusion, 6 months after the start of treatment, about 50% of the patients continued the drug treatment, maintaining the drug compliance of 80% or more, and the factors related to higher compliance to lipid lowering therapy were old age, regular exercise, previous statin therapy, presence of concomitant medication, presence of hypertension or diabetes, and higher CHD risk level. The high LDL cholesterol is a factor related to lower compliance.