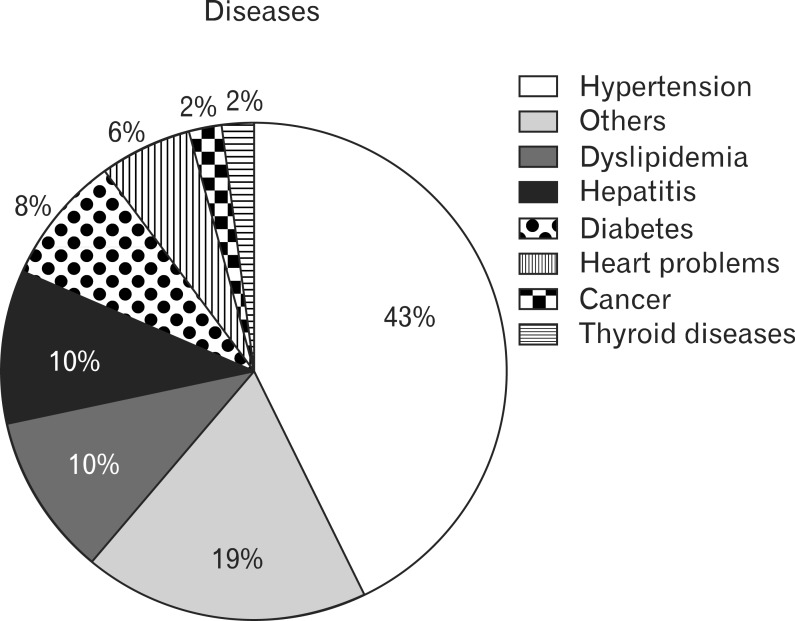
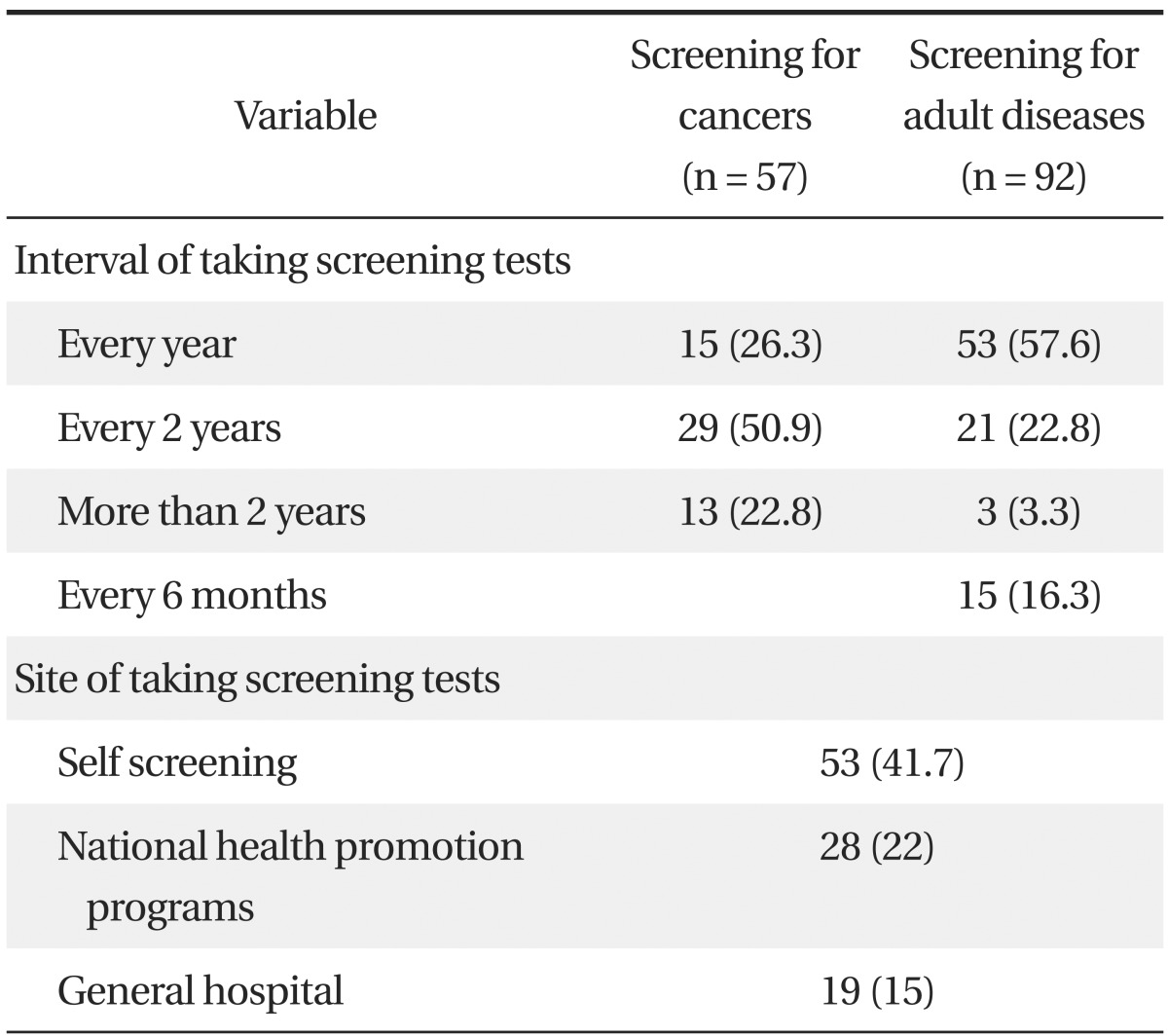
|
 |
- Search
| Korean J Fam Med > Volume 35(1); 2014 > Article |
Abstract
Background
Methods
Results
References
Table 1
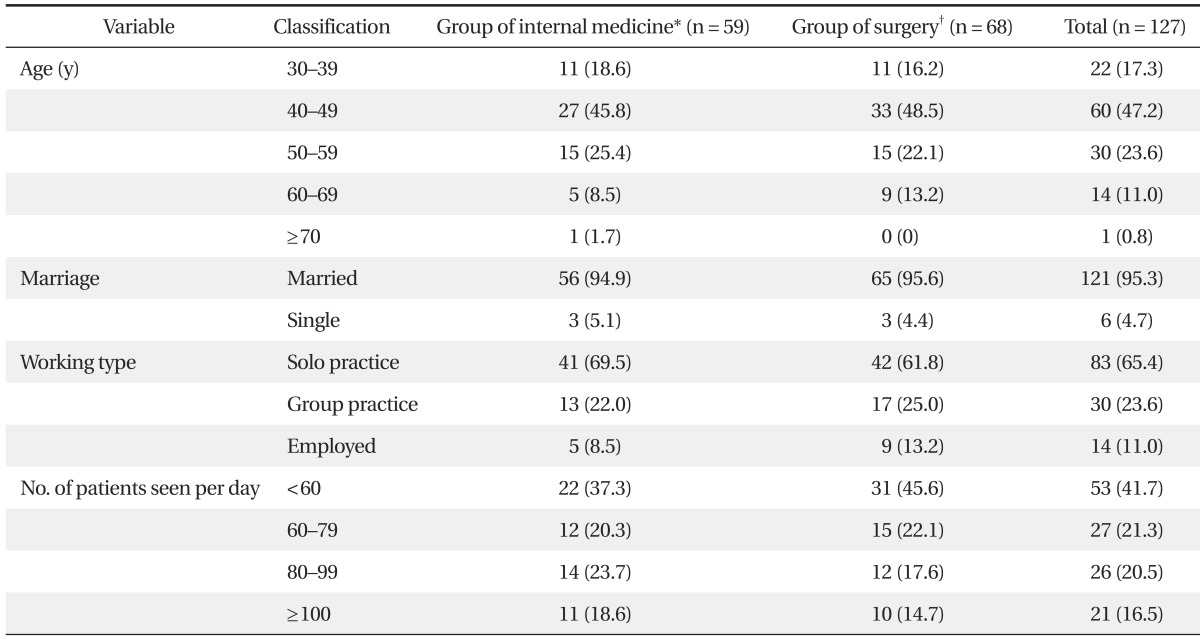
Values are presented as number (%).
*It included family medicines, internal medicine, pediatrics, psychiatry, neurology, dermatology, rehabilitation medicine, radiology, and so on. †It included surgery, orthopedic surgery, neurosurgery, urology, ophthalmology, plastic surgery, thoracic surgery, obstetrics and gynecology, anesthesiology, otolaryngology, and so on.
Table 2
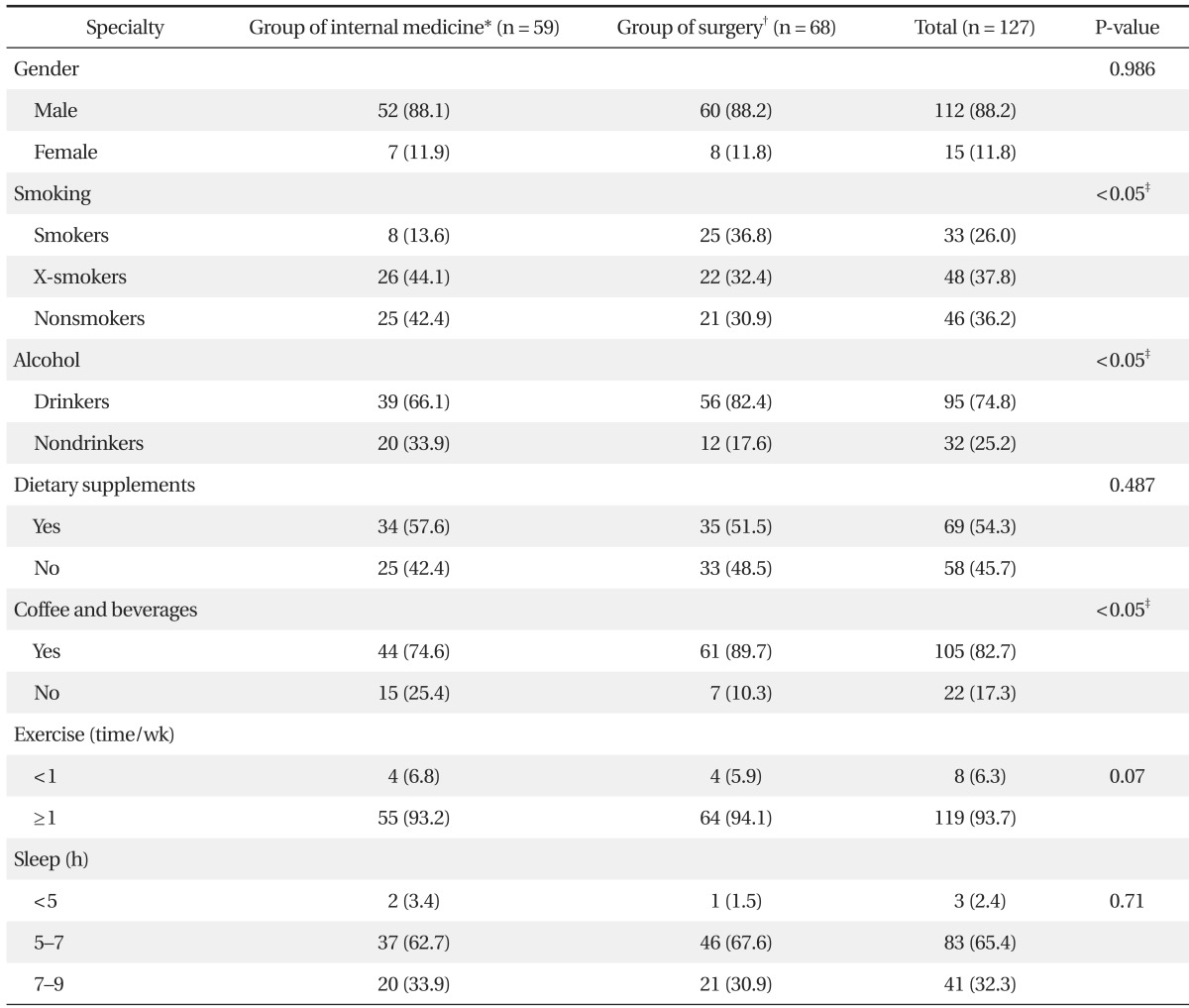
Values are presented as number (%).
*It included family medicines, internal medicine, pediatrics, psychiatry, neurology, dermatology, rehabilitation medicine, radiology, and so on. †It included surgery, orthopedic surgery, neurosurgery, urology, ophthalmology, plastic surgery, thoracic surgery, obstetrics and gynecology, anesthesiology, otolaryngology, and so on. ‡By chi-square test.
Table 4
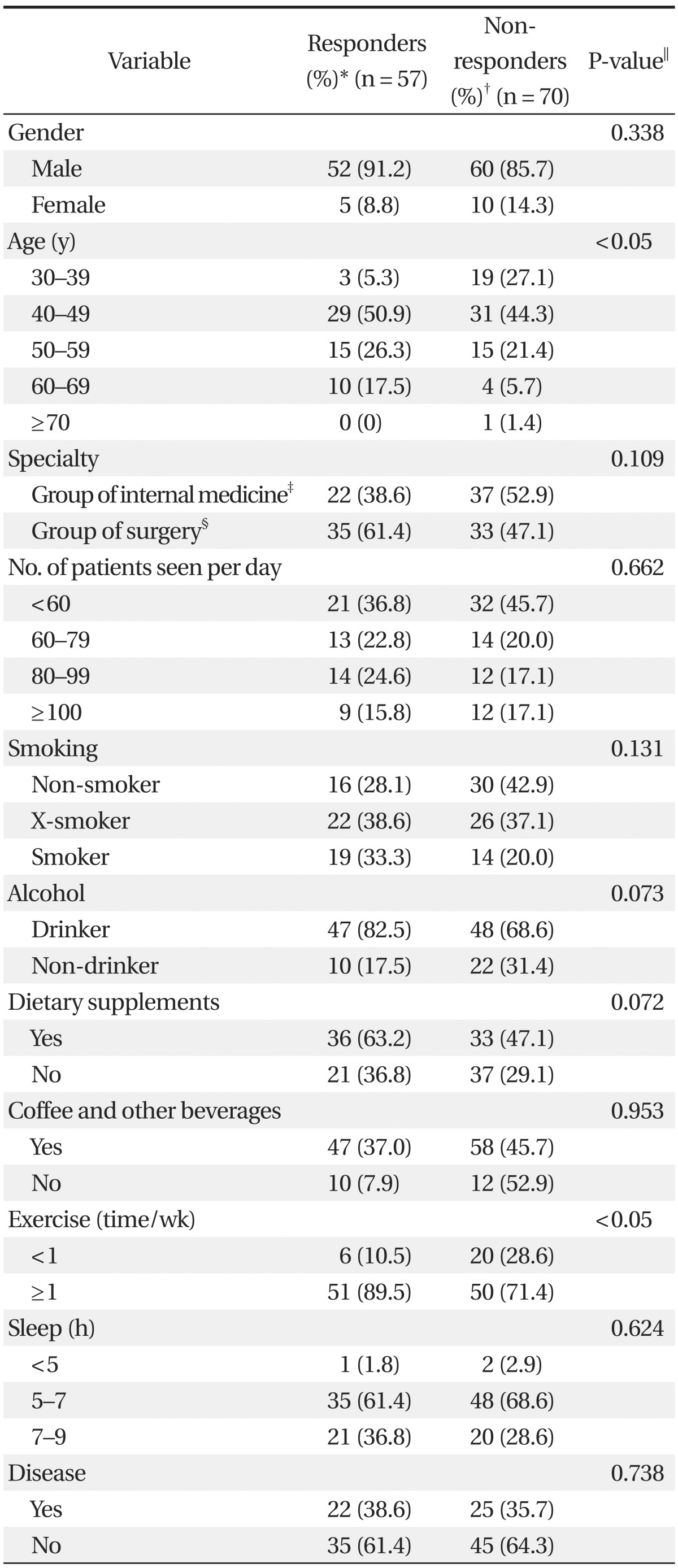
*Responders: participants who performed regular periodic health screening test. †Non-responders: participants who didn't performed regular periodic health screening test. ‡It included family medicines, internal medicine, pediatrics, psychiatry, neurology, dermatology, rehabilitation medicine, radiology, and so on. §It included surgery, orthopedic surgery, neurosurgery, urology, ophthalmology, plastic surgery, thoracic surgery, obstetrics and gynecology, anesthesiology, otolaryngology, and so on. ∥From Fisher's exact test and chi-square test between 2 groups.
Table 5
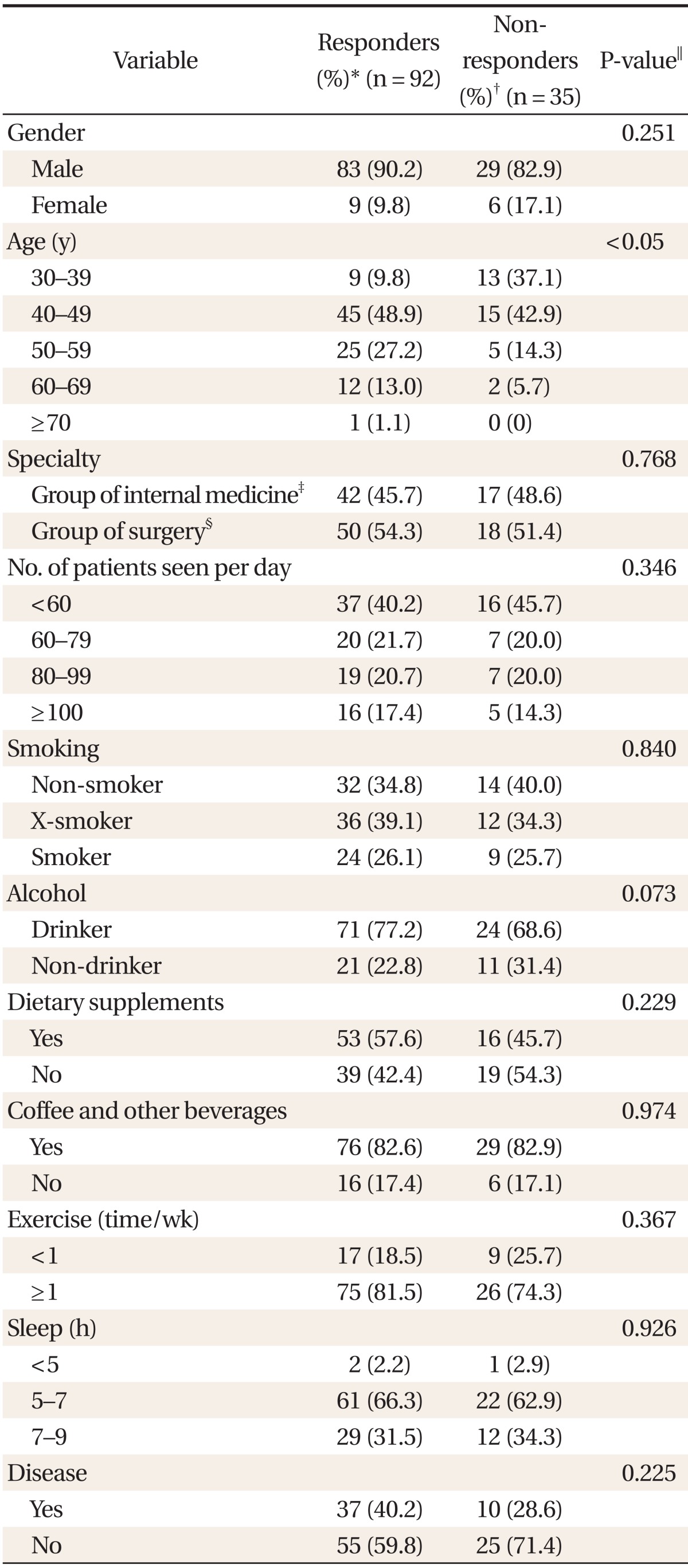
*Responders: participants who performed regular periodic health screening test. †Non-responders: participants who didn't performed regular periodic health screening test. ‡It included family medicines, internal medicine, pediatrics, psychiatry, neurology, dermatology, rehabilitation medicine, radiology, and so on. §It included surgery, orthopedic surgery, neurosurgery, urology, ophthalmology, plastic surgery, thoracic surgery, obstetrics and gynecology, anesthesiology, otorhinolaryngology, and so on. ∥From Fisher's exact test and chi-square test between 2 groups.
- TOOLS