|
 |
- Search
| Korean J Fam Med > Volume 41(4); 2020 > Article |
|
See commentary "Problem Drinking in Cancer Survivors" in Volume 41 on page 205.
Abstract
Background
Problem drinking increases the incidence of all-cause mortality and specific cancers, and persistent drinking is associated with cardiovascular disease in certain cancer survivors. This study analyzed the cardiovascular risk factors before and after diagnosis in Korean cancer survivors.
Methods
Data for the period between 2002 and 2013 were collected from the National Health Insurance Service Health-Examinee Cohort Database. Among the 27,835 patients included, those with moderate alcohol consumption before and after cancer diagnosis were excluded. Problem drinking was defined as males under 65 years consuming over 14 glasses a week, and males over 65 years or females consuming over seven glasses a week. A t-test, chi-square test, and linear regression analysis were performed for differences in cardiovascular risk factors and differences according to cancer types.
Results
There was a difference in the body mass index, systolic and diastolic blood pressure, and total cholesterol among patients who became moderate drinkers after diagnosis, but fasting blood glucose did not show any significant changes. Risk factors for cardiovascular disease were analyzed in patients with liver, stomach, rectal, and breast cancer with improved drinking behavior, and there were significant differences in body mass index, systolic and diastolic blood pressure, fasting blood glucose, and total cholesterol in stomach cancer patients.
Alcohol consumption creates a serious medical and economic burden at the societal level and is associated with deaths from liver disease, cancer, and various chronic diseases at the individual level [1]. Together with smoking, physical activity, and diet, alcohol consumption has a large impact on health. Although the importance of moderation is emphasized, the level of alcohol consumption in South Korea is on the rise [2].
Various organizations in the United States, United Kingdom, the Netherlands, and Australia have suggested guidelines for temperance and healthy drinking [3-5]. According to the World Health Organization (WHO)ŌĆÖs 2014 report, alcohol consumption worldwide is on the rise. As alcohol consumption among females and young age groups, who previously consumed only small amounts, shows a steady increase, South Korea is also making various efforts to promote healthy drinking through a comprehensive citizen health promotion plan [6].
However, alcohol consumption is not all bad. When consumed in moderation, alcohol is effective in preventing mortality from cardiovascular disease (CVD), has cardioprotective effects, and is associated with a relatively reduced risk of myocardial infarction [7]. Furthermore, it has been reported to be effective in decreasing low-density lipoprotein and increasing high-density lipoprotein in regard to lipid metabolism [8]. However, this mechanism is unclear.
Alcohol consumption is also known to have a large impact on the pathogenesis and prognosis of cancer. In particular, oral, pharynx, larynx, esophageal, liver, colon, rectal, and female breast cancer are known to have causal relationships with drinking, and pancreatic and lung cancer are also expected to have associations with drinking [9]. It has been reported that in comparison with non-drinkers, the regular consumption of approximately 50 g of alcohol per day confers a three-fold increased risk of oral and pharyngeal cancers, a 1.5-fold increased risk of female breast cancer, and a 1.4-fold increased risk of colon cancer [10].
Numerous studies have analyzed alcohol consumption and the risk factors for CVD; however, few have investigated the effects drinking behavior improvement before and after a cancer diagnosis among Koreans. Hence, this study intended to investigate CVD-related risk factors among cancer survivors whose drinking behavior changed after a cancer diagnosis and the impact of cardiovascular risk factors in cancers after changes in drinking behavior.
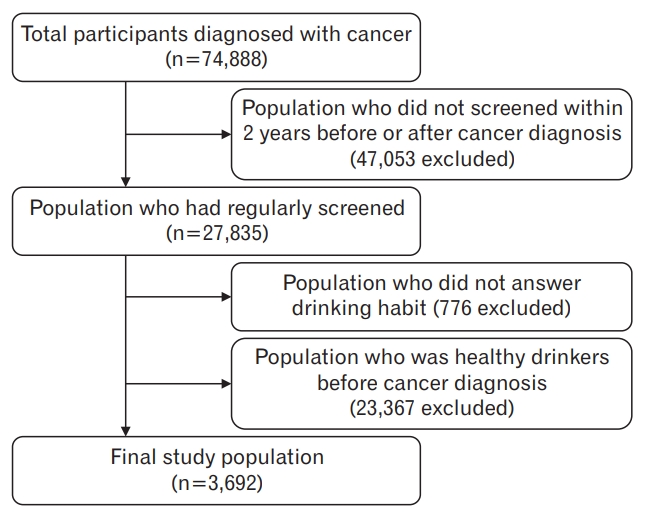
This study used the National Health Insurance Service Health-Examinee Cohort Database (2002ŌĆō2013). Of the 514,866 patients (10% of the initial 5,150,000), 74,888 were diagnosed with cancer. To analyze drinking behavior changes before and after a cancer diagnosis, only examinees who had undergone health examinations within 2 years of the date of cancer diagnosis were included, and examinees whose drinking behavior survey was omitted or who drank moderately before cancer diagnosis were excluded. The final study population for the analysis of CVD-related risk factors with respect to drinking behavior changes comprised a total of 3,692 cancer survivors: 2,495 who showed behavior change to moderate drinking after a cancer diagnosis, and 1,197 who showed no drinking behavior change and continued problem drinking after a cancer diagnosis (Figure 1). Although there was no safe amount of alcohol consumption, the study aim was given to groups that should emphasize lifestyle modification when educating patients. Therefore, it was necessary to study the groups that need intervention first which is why we excluded the groups who were healthy drinkers before the cancer diagnosis. The Seoul National University Bundang Hospital Institutional Review Board (IRB) approved this study (IRB approval no., X-1701/378ŌĆō902) and waived the requirement for informed consent from study participants as the NHIS database is anonymized in adherence to strict confidentiality guidelines. All experiments were performed in accordance with the relevant guidelines and regulations.
The subjectsŌĆÖ past medical history, sociodemographic information, and life habits were collected through a self-administered questionnaire. In this study, age, sex, monthly average household income, body mass index (BMI), smoking, degree of exercise, and past medical history were analyzed as factors that could affect the pathogenesis of CVD and cancer. Examinees aged 40 years or older were grouped together within 10-year intervals. Income was divided into quartiles (Q1ŌĆōQ4) according to age groups. BMI was calculated by dividing body weight by the height squared (weight [kg]/height2 [m2]) and was categorized into underweight (BMI <18.5), normal (18.5Ōēż BMI Ōēż22.9), overweight (23.0Ōēż BMI Ōēż24.9), and obese (BMI Ōēź25.0) according to BMI criteria for the Asian population defined by WHO. Smoking was stratified into ŌĆ£noŌĆØ and ŌĆ£yesŌĆØ according to the experience of smoking. As for the degree of physical activity, it was divided into ŌĆ£insufficientŌĆØ and ŌĆ£sufficient,ŌĆØ with 3 times per week as the criterion.
The groups were divided on the basis of drinking amount, and the criterion for moderate drinking was an average of 14 units of alcohol or below per week for adult males and an average of seven units or below per week for adult females and males aged 65 years or older [11]. ŌĆ£Heavy drinkingŌĆØ refers to a case where the average amount per week exceeds the range of moderate drinking, and ŌĆ£binge drinkingŌĆØ refers to a case where the maximum drinking amount in one session exceeds the range of moderate drinking. Heavy and binge drinking were defined as dangerous drinking. This study used the category of problem drinking, which refers to cases where males under the age of 65 drink more than 14 units of alcohol per week, or males aged 65 years or older or females who drink more than seven units of alcohol per week [12-14].
Individuals who showed improvements in drinking behavior toward moderate drinking after their cancer diagnosis were classified into group 1 and those whose problem drinking persisted after their cancer diagnosis were classified into group 2.
All analyses identified changes in risk factors according to changes in drinking behavior, and the changes were represented as real numbers, means┬▒standard deviation, and percentages. In the comparative analysis of drinking behavior changes after cancer diagnosis and CVD-related risk factors, a Student t-test, chi-square test, and linear regression analysis were conducted. Statistical analysis was additionally adjusted for age, sex, income quantile, smoking, physical activity, and past medical history. Statistics were analyzed using Stata ver. 14.0 (Stata Corp., College Station, TX, USA), and P-values <0.05 were defined as statistically significant.
In this study, 3,692 out of 74,888 patients diagnosed with cancer were included in the final analysis. The number of cases showing behavioral improvements toward moderate drinking after a cancer diagnosis (group 1) was 2,496, and the number of cases showing persistent problem drinking after a cancer diagnosis (group 2) was 1,197. In groups 1 and 2, the average age was 56.6┬▒9.9 years and 55.0┬▒10.2 years, respectively (P<0.001), and the proportion of males was found to be 91.50% and 95.15%, respectively (P<0.001). In addition, the proportion of those with normal BMI was 39.24% in group 1 and 33.00% in group 2 (P=0.001), but there were no intergroup differences in income quintile, physical activity, and past medical history (Table 1). Baseline characteristics for the groups excluded after cancer diagnosis were the same (Supplementary Table 1).
Drinking behavior changes to moderate drinking after a cancer diagnosis resulted in a tendency for the BMI to decline by -0.36┬▒1.68 kg/m2 (P<0.001), systolic blood pressure (SBP) by -5.41┬▒17.64 mm Hg (P<0.001), diastolic blood pressure (DBP) by -3.51┬▒12.28 mm Hg (P<0.001), and total cholesterol (TC) by -6.25┬▒40.42 mg/dL (P=0.007), respectively. This statistical tendency was also observed after the analysis was adjusted for age, sex, income quantile, smoking, physical activity, and past medical history (Table 2).
Among the cancers associated with drinking, patients with liver (P=0.005), stomach (P<0.001), rectal (P=0.002), and breast cancer (P=0.002) showed drinking behavior improvements to moderate drinking after diagnosis, while patients with head and neck, pancreatic, and colorectal cancers showed no drinking behavior improvement (Table 3). Analysis of CVD-related risk factors among patients who showed behavioral improvements to moderate drinking revealed correlations only in stomach cancer cases: with BMI (1.05; 95% CI, 0.69 to 1.41; P<0.001), SBP (9.52; 95% CI, 6.02 to 13.03; P<0.001), DBP (7.16; 95% CI, 4.78 to 9.53; P<0.001), FBS (6.45; 95% CI, 0.42 to 12.49; P=0.036), and TC (16.50; 95% CI, 7.23 to 25.77; P=0.001). In cases of liver, rectal, and breast cancers, no differences were observed in CVD-related risk factors (Table 4).
In a large survey of adult Koreans aged 40 years or older, this study investigated the changes in cardiovascular risk factors among cancer survivors according to changes in their drinking behavior through. By analyzing the cardiovascular risk factors among the existing problem drinking groups according to changes in drinking behavior after a cancer diagnosis, we found associations between drinking and cardiovascular risk factors excluding FBS (Table 2). The results do not differ from the findings of a previous study with 6,413 healthy Koreans that showed changes in SBP and DBP and an increase of FBS [15].
Although previous studies investigated cardiovascular risk factors and the causes of mortality according to specific cancer types, they were limited in terms of research on the effects of drinking behavior improvements after excessive alcohol consumption on CVD and mortality. A recent study of healthy people reported improvements in insulin resistance, blood pressure, and weight, and decreases in growth factors related to cancer after abstaining from drinking for 1 month [16]. However, not much is known about the factors that are influenced by drinking behavioral improvement among cancer survivors.
As head and neck, esophageal, stomach, pancreatic, colorectal, rectal, and breast cancers have associations with alcohol consumption, improvements in drinking behavior was associated with statistically significant differences among patients with stomach, liver, rectal, and breast cancer, along with most other cancers (Table 2). It is presumed that these effects are the result of changes in the perception brought about by a number of studies reporting the direct influence of alcohol consumption on cardiovascular and overall mortality [9,17,18].
There have been reports on cardiovascular risk factors and mortality in patients with various cancers, but reports related to alcohol consumption have been limited. In the case of patients with breast cancer, it is perceived that CVD contributes significantly to the risk of cancer death, and it is reported that death from CVD is related to cardiotoxicity and reduced estrogen [19]. Some studies, however, report that alcohol consumption has no assocaition with mortality in breast cancer survivors [20].
In cases of colorectal and rectal cancer, while some studies on the association between alcohol consumption and carcinogenesis report that there is no connection between them [21], others report that they have some connection [7] and that alcohol affects folic acid metabolism to increase the risk of colorectal cancer [12]. However, research on persistent alcohol consumption and CVD in patients with colorectal cancer has not been conducted.
Excessive alcohol consumption has been known to be a risk factor for hepatocellular carcinoma, and it is reported that its incidence has a positive correlation with the amount of drinking [9,18]. It has been reported that the mechanism for hepatocarcinogenesis caused by alcohol is related to carcinogen metabolism in the liver as well as the development of liver cirrhosis [22]. However, its association with CVD has not been clearly reported.
In cases of stomach cancer, there is no consistent evidence regarding the effects of alcohol consumption. While some studies report that the risk of stomach cancer increases as the amount of alcohol intake increases [23], others report that there is no difference [21].
The biological mechanism common to CVD and cancer caused by alcohol consumption is chronic inflammation [10]. Excessive alcohol intake increases mortality, the incidence of CVD, neutral fat, hypertension, atrial fibrillation, cardiomyopathy, and stroke, and in this process, comes to have various effects on inflammation, platelet aggregation, myocardial ischemia reperfusion, coagulation factors, vascular endothelial cell function, and anti-apoptotic pathways [17,22]. In terms of carcinogenesis, acetaldehyde, a primary product of alcohol metabolism, has toxic effects, accelerating the production of reactive oxygen and nitrogen species to impact folate and methionine metabolism and DNA repair mechanisms, causing the development of cancerous cells [16,23].
The limitations of this study are as follows. First, it is probable that the subjectsŌĆÖ subjective opinions were included because their lifestyle habits were collected through a self-administered questionnaire. Second, since the subjects of this study were people who underwent regular national health examinations and were interested in maintaining their health, it is possible that they showed better improvements in lifestyle habits than the ordinary populations would have. Third, while it was confirmed that changes in drinking behavior were associated with cardiovascular risk factors, whether changes in drinking behavior can affect overall mortality, and more specifically, CVD mortality, could not be elucidated. Fourth, QRISK and Framingham risk scores are used to determine an individualŌĆÖs cardiovascular risk, but in performing the analysis using the National Health Insurance Service Health-Examinee Cohort Database, there were limitations in using those data.
In conclusion, it was found that excessive alcohol consumption of Korean cancer survivors increased the risk factors associated with CVD and that drinking behavior improvements after a cancer diagnosis decreased the risk factors associated with CVD. Therefore, it is necessary to conduct research on what effects these changes have on mortality.
SUPPLEMENTARY MATERIALS
Supplementary materials can be found via https://doi.org/10.4082/kjfm.18.0119. Supplementary Table 1. Baseline characteristics of the
exclusion population.
Table┬Ā1.
Baseline characteristics of study population (n=3,692)
| Characteristic | Group 1 | Group 2 | Total | P-value* |
|---|---|---|---|---|
| Total | 2,495 | 1,197 | 3,692 | |
| Age (y) | <0.001 | |||
| ŌĆā40ŌĆō49 | 755 (30.26) | 474 (39.60) | 1,229 (33.29) | |
| ŌĆā50ŌĆō59 | 708 (28.38) | 360 (25.56) | 1,014 (27.46) | |
| ŌĆā60ŌĆō69 | 769 (30.82) | 291 (24.31) | 1,060 (28.71) | |
| ŌĆāŌēź70 | 263 (10.54) | 126 (10.53) | 389 (10.54) | |
| Sex | <0.001 | |||
| ŌĆāMale | 2,283 (91.50) | 1,139 (95.15) | 3,422 (92.69) | |
| ŌĆāFemale | 212 (8.50) | 58 (4.85) | 270 (7.31) | |
| Income | 0.053 | |||
| ŌĆāQuartile 1 | 858 (34.39) | 360 (30.08) | 1,218 (32.99) | |
| ŌĆāQuartile 2 | 441 (17.68) | 226 (18.88) | 667 (18.07) | |
| ŌĆāQuartile 3 | 699 (28.02) | 371 (30.99) | 1,070 (28.98) | |
| ŌĆāQuartile 4 | 497 (19.92) | 240 (20.05) | 737 (19.96) | |
| Body mass indexŌĆĀ | 0.001 | |||
| ŌĆā<18.5 | 82 (3.29) | 25 (2.09) | 107 (2.90) | |
| ŌĆā18.5ŌĆō22.9 | 897 (35.95) | 370 (30.91) | 1,267 (34.32) | |
| ŌĆā23.0ŌĆō24.9 | 641 (25.69) | 346 (28.91) | 987 (26.73) | |
| ŌĆāŌēź25.0 | 875 (35.07) | 456 (38.10) | 1,331 (36.05) | |
| Smoking | <0.001 | |||
| ŌĆāYes | 874 (36.85) | 321 (28.16) | 1,195 (34.03) | |
| ŌĆāNo | 1,498 (63.15) | 819 (71.84) | 2,317 (65.97) | |
| Physical activity | 0.743 | |||
| ŌĆāInsufficient | 1,553 (62.24) | 752 (62.82) | 2,305 (62.43) | |
| ŌĆāSufficient | 942 (37.76) | 445 (37.18) | 1,387 (37.57) | |
| Past medical history | ||||
| ŌĆāHypertension | 441 (17.68) | 241 (20.13) | 682 (18.47) | 0.072 |
| ŌĆāDiabetes mellitus | 201 (8.06) | 98 (8.19) | 299 (8.10) | 0.891 |
| ŌĆāStroke | 15 (0.60) | 8 (0.67) | 23 (0.62) | 0.808 |
| ŌĆāCardiovascular disease | 48 (1.92) | 25 (2.09) | 73 (1.98) | 0.737 |
Table┬Ā2.
Linear regression analysis of CVD risk factors
| Variable |
Mean┬▒standard deviation |
Crude analysis |
Adjusted analysis* |
||||
|---|---|---|---|---|---|---|---|
| Before diagnosis | After diagnosis | Change | Coef. (95% CI) | P-value | Coef. (95% CI) | P-value | |
| BMI | 0.41 (0.30 to 0.52) | <0.001 | 0.43 (0.32 to 0.54) | <0.001 | |||
| ŌĆāGroup 1 | 23.81┬▒2.91 | 23.45┬▒2.97 | -0.36┬▒1.68 | ||||
| ŌĆāGroup 2 | 24.27┬▒3.01 | 24.32┬▒3.13 | 0.05┬▒1.29 | ||||
| Systolic blood pressure | 3.59 (2.36 to 4.81) | <0.001 | 3.65 (2.38 to 4.91) | <0.001 | |||
| ŌĆāGroup 1 | 130.07┬▒16.43 | 124.65┬▒15.08 | -5.41┬▒17.64 | ||||
| ŌĆāGroup 2 | 130.07┬▒15.90 | 128.77┬▒15.31 | -1.82┬▒17.89 | ||||
| Diastolic blood pressure | 2.01 (1.18 to 2.84) | <0.001 | 2.02 (1.16 to 2.88) | <0.001 | |||
| ŌĆāGroup 1 | 80.64┬▒10.54 | 77.12┬▒10.06 | -3.51┬▒12.28 | ||||
| ŌĆāGroup 2 | 81.19┬▒10.60 | 79.70┬▒9.93 | -1.50┬▒11.61 | ||||
| Fasting blood sugar | 1.56 (-0.71 to 3.94) | 0.178 | 1.55 (-0.82 to -3.92) | 0.199 | |||
| ŌĆāGroup 1 | 105.19┬▒34.32 | 104.43┬▒31.91 | -0.75┬▒32.76 | ||||
| ŌĆāGroup 2 | 106.17┬▒35.86 | 107.00┬▒28.94 | 0.82┬▒33.41 | ||||
| Total cholesterol | 3.80 (1.05 to 6.55) | 0.007 | 3.94 (1.09 to 6.79) | 0.007 | |||
| ŌĆāGroup 1 | 193.29┬▒40.00 | 187.05┬▒37.14 | -6.25┬▒40.42 | ||||
| ŌĆāGroup 2 | 192.42┬▒39.19 | 188.94┬▒39.97 | -2.45┬▒38.86 | ||||
Table┬Ā3.
Prevalence of cancer in relation to changing drinking habits
| Cancer | Total | Group 1 | Group 2 | P-value* |
|---|---|---|---|---|
| Liver cancer | 473 | 293 (61.95) | 180 (38.05) | 0.005 |
| Pancreatic cancer | 106 | 71 (66.98) | 35 (35.02) | 0.894 |
| Hepatobiliary cancer | 47 | 32 (68.09) | 15 (31.91) | 0.940 |
| Stomach cancer | 592 | 465 (78.55) | 127 (21.45) | <0.001 |
| Colon cancer | 350 | 225 (64.29) | 125 (35.71) | 0.167 |
| Rectal cancer | 168 | 132 (78.57) | 36 (21.43) | 0.002 |
| Lung cancer | 313 | 204 (65.18) | 109 (34.82) | 0.342 |
| Thyroid cancer | 180 | 125 (69.44) | 55 (30.56) | 0.583 |
| Breast cancer | 35 | 32 (91.43) | 3 (8.57) | 0.002 |
| Prostate cancer | 624 | 379 (60.74) | 245 (39.26) | <0.001 |
| Hematologic cancer | 50 | 38 (76.00) | 12 (24.00) | 0.200 |
| Bladder cancer | 109 | 73 (66.97) | 36 (33.03) | 0.891 |
| Renal cancer | 77 | 52 (67.53) | 25 (32.47) | 0.993 |
| Esophageal cancer | 35 | 27 (77.14) | 8 (22.86) | 0.225 |
| Laryngeal cancer | 177 | 114 (64.41) | 63 (35.59) | 0.356 |
Table┬Ā4.
Linear regression analysis of CVD risk factors by cancer type
| Variable | Category |
Liver cancer |
Stomach cancer |
Rectal cancer |
Breast cancer |
||||
|---|---|---|---|---|---|---|---|---|---|
| Coef. (95% CI) | P-value | Coef. (95% CI) | P-value | Coef. (95% CI) | P-value | Coef. (95% CI) | P-value | ||
| BMI | Crude | 0.11 (-0.17 to 0.38) | 0.442 | 1.05 (0.69 to 1.41) | <0.001 | 0.01 (-0.57 to 0.60) | 0.961 | 0.55 (-1.38 to 2.47) | 0.567 |
| Adjusted* | 0.16 (-0.13 to 0.45) | 0.276 | 0.97 (0.61 to 1.34) | <0.001 | -0.11 (-0.70 to 0.47) | 0.707 | 0.60 (-1.49 to 2.69) | 0.560 | |
| Systolic blood pressure | Crude | 2.54 (-0.89 to 5.96) | 0.146 | 9.52 (6.02 to 13.03) | <0.001 | 3.58 (-2.21 to 9.38) | 0.224 | -6.36 (-24.61 to 11.88) | 0.483 |
| Adjusted | 2.42 (-1.17 to 6.01) | 0.186 | 9.40 (5.84 to 12.96) | <0.001 | 3.45 (-2.94 to 9.84) | 1.070 | -5.31 (-29.66 to 19.03) | 0.658 | |
| Diastolic blood pressure | Crude | 1.25 (-1.08 to 3.59) | 0.292 | 7.16 (4.78 to 9.53) | <0.001 | 1.87 (-2.14 to 5.88) | 0.358 | -1.55 (-13.81 to 10.71) | 0.798 |
| Adjusted | 1.39 (-1.09 to 3.86) | 0.271 | 6.93 (4.48 to 9.38) | <0.001 | 1.83 (-2.28 to 5.94) | 0.380 | 0.14 (-14.74 to 15.02) | 0.984 | |
| Fasting blood sugar | Crude | 5.47 (-3.29 to 14.23) | 0.220 | 6.45 (0.42 to 12.49) | 0.036 | 2.15 (-4.96 to 9.25) | 0.551 | -7.32 (-22.22 to 7.58) | 0.325 |
| Adjusted | 6.71 (-2.77 to 16.18) | 0.165 | 4.38 (-1.84 to 10.60) | 0.167 | 2.37 (-5.35 to 10.08) | 0.545 | -10.14 (-29.18 to 8.90) | 0.284 | |
| Total cholesterol | Crude | -4.59 (-12.38 to 3.20) | 0.247 | 16.50 (7.23 to 25.77) | 0.001 | 6.38 (-6.08 to 18.84) | 0.313 | -3.64 (-52.40 to 45.14) | 0.880 |
| Adjusted | -2.02 (-10.28 to 6.24) | 0.631 | 16.57 (6.87 to 26.28) | 0.001 | 6.62 (-6.57 to 19.80) | 0.323 | -18.25 (-79.61 to 43.10) | 0.547 | |
REFERENCES
1. Xi B, Veeranki SP, Zhao M, Ma C, Yan Y, Mi J. Relationship of alcohol consumption to all-cause, cardiovascular, and cancer-related mortality in U.S. adults. J Am Coll Cardiol 2017;70:913-22.


2. Park H. Prevalence and related risk factors of problem drinking in Korean adult population. J Korea Acad Ind Coop Soc 2018;19:389-97.
3. Health Council of the Netherlands. Work programme 2017. The Hague: Health Council of the Netherlands;; 2016.
4. Guirguis-Blake J, Calonge N, Miller T, Siu A, Teutsch S, Whitlock E, et al. Current processes of the U.S. Preventive Services Task Force: refining evidence-based recommendation development. Ann Intern Med 2007;147:117-22.


5. Park JE, Kim HN, Kim KH, Kim H. Development of lifestyle disease guidelines and the role of physicians. J Korean Med Assoc 2018;61:62-70.

6. Rothe D, Paterson I, Cox-Kennett N, Gyenes G, Pituskin E. Prevention of cardiovascular disease among cancer survivors: the role of pre-existing risk factors and cancer treatments. Curr Epidemiol Rep 2017;4:239-47.


7. Yoon YS, Oh SW, Baik HW, Park HS, Kim WY. Alcohol consumption and the metabolic syndrome in Korean adults: the 1998 Korean National Health and Nutrition Examination Survey. Am J Clin Nutr 2004;80:217-24.



9. Koene RJ, Prizment AE, Blaes A, Konety SH. Shared risk factors in cardiovascular disease and cancer. Circulation 2016;133:1104-14.



10. Kim JS. Management of drinking patients in primary care. Korean J Fam Pract 2012;2:280-8.
11. Harris KC, Benoit G, Dionne J, Feber J, Cloutier L, Zarnke KB, et al. Hypertension CanadaŌĆÖs 2016 Canadian Hypertension Education Program guidelines for blood pressure measurement, diagnosis, and assessment of risk of pediatric hypertension. Can J Cardiol 2016;32:589-97.


12. Willenbring ML, Massey SH, Gardner MB. Helping patients who drink too much: an evidence-based guide for primary care clinicians. Am Fam Physician 2009;80:44-50.

13. Lee CT. Medical aspects on moderate drinking. J Korean Public Health Assoc 2000;26:373-82.
14. Park SH, Kang YH, Park HY. Alcohol consumption and the coronary heart disease-related risk factors in Korean adults: the third Korea National Health and Nutrition Examination Survey (KNHANES III), 2005. Korean J Nutr 2008;41:232-41.
15. Mehta G, Macdonald S, Cronberg A, Rosselli M, Khera-Butler T, Sumpter C, et al. Short-term abstinence from alcohol and changes in cardiovascular risk factors, liver function tests and cancer-related growth factors: a prospective observational study. BMJ Open 2018;8:e020673.



16. Bagnardi V, Rota M, Botteri E, Tramacere I, Islami F, Fedirko V, et al. Light alcohol drinking and cancer: a meta-analysis. Ann Oncol 2013;24:301-8.



17. Costanzo S, Di Castelnuovo A, Donati MB, Iacoviello L, de Gaetano G. Cardiovascular and overall mortality risk in relation to alcohol consumption in patients with cardiovascular disease. Circulation 2010;121:1951-9.


18. Corrao G, Bagnardi V, Zambon A, La Vecchia C. A meta-analysis of alcohol consumption and the risk of 15 diseases. Prev Med 2004;38:613-9.


19. Tu H, Wen CP, Tsai SP, Chow WH, Wen C, Ye Y, et al. Cancer risk associated with chronic diseases and disease markers: prospective cohort study. BMJ 2018;360:k134.



20. Newcomb PA, Kampman E, Trentham-Dietz A, Egan KM, Titus LJ, Baron JA, et al. Alcohol consumption before and after breast cancer diagnosis: associations with survival from breast cancer, cardiovascular disease, and other causes. J Clin Oncol 2013;31:1939-46.



21. Franceschi S, La Vecchia C. Alcohol and the risk of cancers of the stomach and colon-rectum. Dig Dis 1994;12:276-89.


- TOOLS